Advanced Cardiothoracic Care by Dr. Asher George Joseph
When a patient has both a serious heart valve condition and a recently transplanted kidney, the treatment approach requires exceptional planning, precision, and teamwork. Heart surgery in such patients is more complex because the medical team must not only correct the heart problem but also protect the newly transplanted kidney and reduce the risk of complications.
This case involved a 52-year-old gentleman who presented with difficulty in breathing. After detailed evaluation, his echocardiogram showed that he had severe aortic valve stenosis. This means that the aortic valve, one of the most important valves in the heart, had become severely narrowed, making it difficult for blood to flow properly from the heart to the rest of the body.
What made this case particularly challenging was that the patient had undergone a renal transplant just ten months earlier. He was on immunosuppressant medications, including steroids, to protect his transplanted kidney. These medicines are essential after a kidney transplant, but they can also increase the risk of infection and delay wound healing after major surgery.
After extensive evaluation and multiple discussions with the nephrology and urology teams, the decision was made to proceed with minimal access aortic valve replacement.
About Dr. Asher George Joseph
Dr. Asher George Joseph is a highly skilled cardiothoracic and transplant surgeon with advanced training in complex heart and transplant-related procedures.
Qualifications:
MBBS, M.Ch CTVS Gold Medalist, MRCS Edinburgh, FACS USA, Fellowship in CT Transplantation and Mechanical Circulatory Support, Manchester, UK
He is regarded as one of the youngest cardiothoracic transplant surgeons and has more than 10 years of experience in managing advanced cardiac surgical cases. His expertise includes cardiothoracic surgery, transplant-related cardiac care, mechanical circulatory support, and complex valve surgeries.
For patients in Bangalore, access to advanced cardiothoracic surgical expertise is especially important when dealing with high-risk heart conditions such as severe aortic stenosis, heart failure, valve disease, and transplant-related cardiac complications.
Understanding Aortic Valve Stenosis
The aortic valve controls blood flow from the heart’s main pumping chamber, the left ventricle, into the aorta, which supplies blood to the entire body. In aortic valve stenosis, this valve becomes narrowed and stiff.
When the valve becomes severely stenosed, the heart has to work much harder to pump blood. Over time, this can lead to symptoms such as:
- Difficulty in breathing
- Chest discomfort
- Fatigue
- Dizziness or fainting
- Reduced exercise capacity
- Heart failure symptoms
In this patient’s case, the primary symptom was difficulty in breathing. The echocardiogram confirmed that the aortic valve was severely narrowed and required surgical treatment.
Why This Case Was More Complex
Aortic valve replacement is a well-established treatment for severe aortic stenosis. However, in this case, the patient had a newly transplanted kidney. This changed the risk profile significantly.
A patient who has undergone renal transplant is usually on immunosuppressant medications. These medicines reduce the body’s immune response so that the transplanted kidney is not rejected. However, they also make surgery more delicate because they can affect:
- Wound healing
- Infection risk
- Recovery speed
- Kidney function
- Response to surgical stress
The medical team had to ensure that the heart surgery was performed safely while protecting the transplanted kidney.
Another important concern was the use of the heart-lung machine during aortic valve surgery. During valve replacement, the patient is usually placed on cardiopulmonary bypass, commonly known as the heart-lung machine. While this is necessary for many cardiac surgeries, it can sometimes affect kidney function, especially in high-risk patients.
Because this patient had received a kidney transplant only ten months earlier, protecting kidney function during and after surgery was a major priority.
Why Minimal Access Aortic Valve Replacement Was Chosen
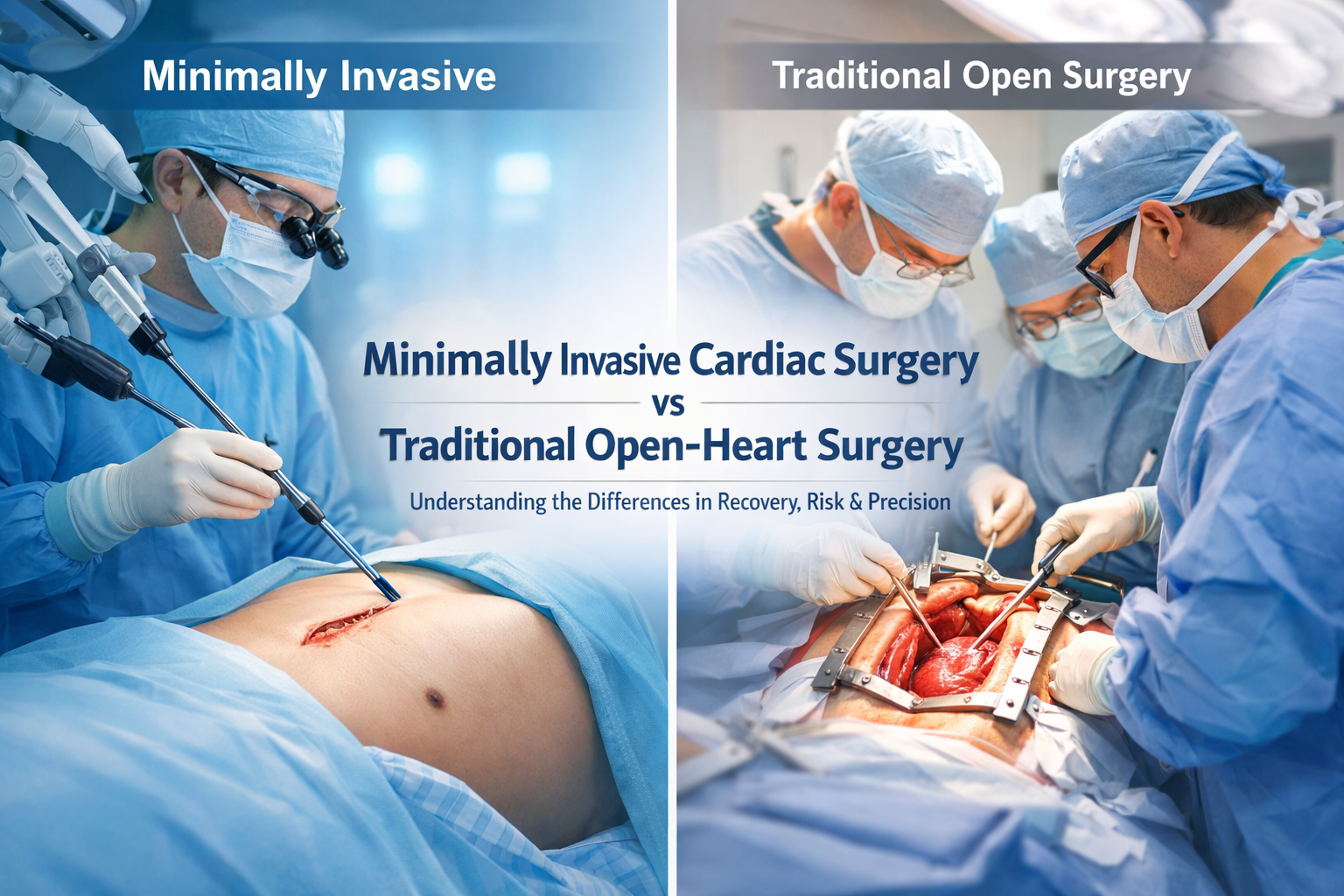
Traditional open-heart surgery often involves cutting through the breastbone to access the heart. While this approach is effective, it can involve a larger incision and more bone healing after surgery.
In this case, the patient was on immunosuppressants and steroids. Since wound healing can be slower in such patients, a traditional larger surgical approach could have increased the risk of delayed healing or wound-related complications.
That is why the surgical team chose a minimal access approach.
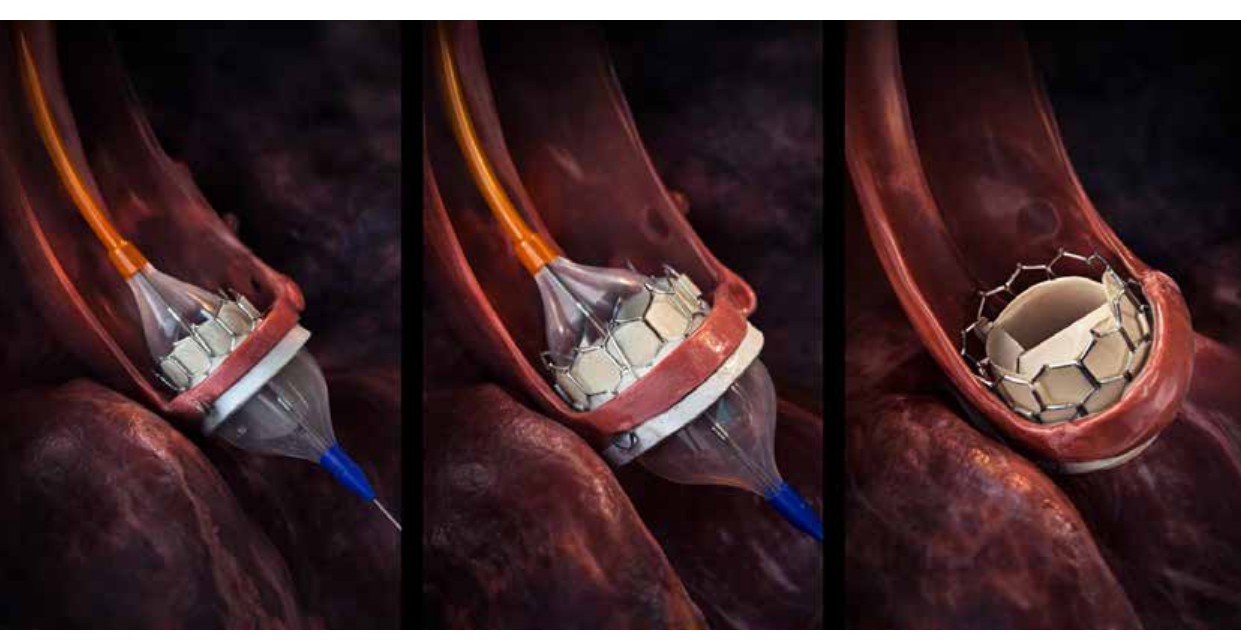
Minimal access aortic valve replacement allows the surgeon to replace the diseased valve through a smaller incision, reducing the amount of bone that needs to be cut. This approach can help support better healing, reduce surgical trauma, and potentially improve recovery in carefully selected patients.
For this patient, the goal was clear:
To replace the severely stenosed aortic valve while minimizing surgical trauma and protecting the newly transplanted kidney.
The Role of Multidisciplinary Planning
One of the most important aspects of this case was the collaborative decision-making process. Before proceeding with surgery, the patient underwent extensive evaluation. The case was discussed with the nephrologist and urologist to assess the risks and plan the safest possible approach.
In complex patients, especially those with a transplant history, surgery is never just about one organ. The heart, kidney, immune system, medications, and overall recovery all need to be considered together.
This type of multidisciplinary approach is especially valuable in advanced cardiac care. It ensures that every important factor is evaluated before surgery, during surgery, and throughout recovery.
Protecting the Transplanted Kidney During Heart Surgery
One of the key challenges in this case was kidney protection. During aortic valve replacement, the heart-lung machine supports circulation while the surgeon works on the valve. However, patients with kidney disease or recent kidney transplantation may have a higher risk of kidney dysfunction after such procedures.
In this patient, the kidney was newly grafted and needed careful protection. The surgical and medical teams had to manage fluid balance, blood pressure, circulation, medications, and postoperative monitoring with great care.
The success of the surgery was not only measured by the replacement of the valve but also by how well the transplanted kidney was protected during the entire process.
Recovery After Minimal Access Aortic Valve Replacement
Following the procedure, the patient made a slow but steady recovery. This is expected in complex cases where the body has already undergone a major transplant procedure in the recent past.
The important outcome was that the patient recovered gradually and was doing well after surgery. For the surgical team, this was a deeply gratifying case because it involved balancing multiple high-risk factors and achieving a successful outcome.
The case highlights how advanced surgical planning, minimal access techniques, and multidisciplinary care can make a major difference in complex heart patients.
Why This Case Matters for Patients in Bangalore
Bangalore is home to many patients seeking advanced treatment for heart valve disease, heart failure, and transplant-related complications. As medical care becomes more advanced, patients are living longer after kidney transplants and other major procedures. However, some of these patients may later develop serious cardiac conditions that require surgical intervention.
For such patients, the treatment approach must be highly individualized.
This case demonstrates that even high-risk patients with recent renal transplantation can be considered for advanced cardiac surgery when the procedure is planned carefully and performed by an experienced cardiothoracic surgical team.
Patients in Bangalore who have symptoms such as breathlessness, chest discomfort, unexplained fatigue, or known valve disease should not delay evaluation. Early diagnosis can help doctors plan the right treatment before the condition becomes more severe.
When Should Aortic Valve Replacement Be Considered?
Aortic valve replacement may be recommended when the valve is severely narrowed and symptoms begin to affect daily life. Breathlessness, fatigue, fainting episodes, and reduced physical capacity are important warning signs.
In severe aortic stenosis, medicines may help control some symptoms temporarily, but they cannot open the narrowed valve. Once the valve becomes critically narrowed, replacement may be necessary to restore proper blood flow and reduce the strain on the heart.
The choice of treatment depends on the patient’s age, health condition, surgical risk, valve anatomy, kidney function, and other medical factors.
In this case, because the patient had severe aortic stenosis and symptoms, valve replacement became necessary despite the complexity of his recent kidney transplant.
Benefits of a Minimal Access Approach in Selected Patients
Minimal access cardiac surgery is not suitable for every patient, but in selected cases, it can offer important advantages.
Potential benefits may include:
- Smaller incision
- Less bone disruption
- Better wound healing support
- Reduced surgical trauma
- Faster mobilization in suitable patients
- Improved comfort during recovery
- Lower wound-related concerns in high-risk patients
For patients on immunosuppressants and steroids, reducing wound-related complications is especially important. This was one of the main reasons minimal access surgery was chosen in this case.
Expert Heart Valve Surgery in Bangalore
Complex heart valve disease requires careful diagnosis, expert surgical planning, and individualized treatment. This is especially true when patients have additional medical challenges such as kidney transplant, immune suppression, diabetes, kidney dysfunction, or previous major surgeries.
Dr. Asher George Joseph’s training in cardiothoracic surgery, transplant surgery, and mechanical circulatory support allows him to approach such cases with advanced clinical understanding.
For patients in Bangalore, this case serves as an important reminder that high-risk cardiac surgery requires not only technical expertise but also thoughtful planning and a strong multidisciplinary approach.
FAQs
1. What is aortic valve stenosis?
Aortic valve stenosis is a condition in which the aortic valve becomes narrowed and stiff. This makes it difficult for blood to flow from the heart to the rest of the body, causing symptoms such as breathlessness, fatigue, chest pain, dizziness, or fainting.
2. Why does severe aortic stenosis require surgery?
When aortic stenosis becomes severe and symptoms develop, the heart has to work harder to pump blood. Over time, this can lead to heart failure and serious complications. In such cases, aortic valve replacement may be required.
3. What is minimal access aortic valve replacement?
Minimal access aortic valve replacement is a surgical technique where the valve is replaced through a smaller incision instead of a full traditional open-heart incision. It helps reduce surgical trauma and may support better recovery in selected patients.
4. Why was minimal access surgery important in this renal transplant patient?
The patient was on immunosuppressants and steroids after a kidney transplant. These medicines can delay wound healing and increase infection risk. A minimal access approach helped reduce bone disruption and supported better healing.
5. Is heart surgery risky after kidney transplant?
Heart surgery after kidney transplant can be more complex because the transplanted kidney must be protected during and after surgery. However, with careful planning, multidisciplinary care, and expert surgical management, selected patients can undergo successful cardiac surgery.
6. Why is kidney protection important during aortic valve surgery?
Aortic valve surgery often requires the use of a heart-lung machine. In patients with kidney disease or recent kidney transplantation, there may be a higher risk of kidney dysfunction. Careful monitoring and planning are essential to protect kidney function.
7. Who is Dr. Asher George Joseph?
Dr. Asher George Joseph is a cardiothoracic and transplant surgeon with qualifications including MBBS, M.Ch CTVS Gold Medalist, MRCS Edinburgh, FACS USA, and fellowship training in CT Transplantation and Mechanical Circulatory Support from Manchester, UK. He has over 10 years of experience.
8. When should patients in Bangalore consult a heart valve surgeon?
Patients should consult a heart valve specialist if they experience breathlessness, chest discomfort, fainting, fatigue, or if an echocardiogram shows valve narrowing or leakage. Early evaluation can help determine the right treatment plan.
9. Can all patients undergo minimal access valve surgery?
No. Minimal access surgery depends on the patient’s anatomy, overall health, valve condition, previous surgeries, and surgical risk. The decision is made after detailed evaluation by the cardiac surgical team.
10. What makes this case a successful outcome?
This case was successful because the severely narrowed aortic valve was replaced using a minimal access approach while carefully protecting the patient’s recently transplanted kidney. The patient made a gradual recovery and was doing well after surgery.